Heart palpitations during perimenopause — a racing, fluttering, or pounding heartbeat — are surprisingly common and usually harmless, though they can be frightening. Fluctuating estrogen directly affects the heart's electrical conduction system, and about 25-40% of perimenopausal women experience palpitations at some point during the transition. Here is what the research says about why they happen, when you should be concerned, and what helps.
This article is for informational purposes only and is not medical advice. If you experience heart palpitations, consult your healthcare provider for proper evaluation.
Why does perimenopause cause heart palpitations?
Your heart has estrogen receptors, and estrogen influences the heart's electrical system, blood vessel tone, and autonomic nervous system. During perimenopause, estrogen levels do not simply decline gradually — they fluctuate wildly, sometimes spiking higher than premenopausal levels before crashing. These rapid hormonal shifts can temporarily affect heart rhythm.
Research published in the journal Menopause has identified several mechanisms linking perimenopause to palpitations:
- Autonomic nervous system changes. Estrogen helps regulate the balance between the sympathetic (fight-or-flight) and parasympathetic (rest-and-digest) nervous systems. Fluctuating estrogen can tip this balance toward sympathetic dominance, increasing heart rate and causing the sensation of palpitations.
- Vasomotor instability. The same mechanism that causes hot flashes — disruption of the hypothalamic thermostat — also triggers surges in adrenaline that can make your heart race.
- Anxiety amplification. Hormonal changes increase anxiety sensitivity, and anxiety itself triggers palpitations, creating a feedback loop.
- Sleep disruption. Poor sleep increases cortisol and adrenaline, both of which affect heart rate and rhythm.
What do perimenopause heart palpitations feel like?
Women describe perimenopause-related palpitations in different ways:
- A sudden awareness of your heartbeat
- Feeling like your heart is racing or beating too fast
- A fluttering sensation in your chest
- A pounding or thumping heartbeat you can feel in your neck or throat
- Skipped beats or a "flip-flopping" sensation
- Brief episodes lasting seconds to minutes
Palpitations often occur at specific times: during or after a hot flash, at night (especially in the early morning hours), during periods of stress, or around the time of your period. Some women notice a clear pattern tied to their menstrual cycle, with palpitations increasing when estrogen drops in the late luteal phase.
How do perimenopause palpitations differ from heart problems?
The anxiety around heart palpitations is understandable — your heart is involved, and it feels urgent. However, most perimenopause-related palpitations are benign premature atrial contractions (PACs) or premature ventricular contractions (PVCs), which are extra heartbeats that feel like a flutter or skipped beat. These are not dangerous.
That said, palpitations can sometimes indicate an underlying cardiac issue. You should seek medical evaluation if you experience:
- Palpitations accompanied by chest pain or tightness
- Shortness of breath during palpitations
- Dizziness, lightheadedness, or fainting during palpitations
- Palpitations that last more than a few minutes
- A resting heart rate consistently above 100 bpm
- Palpitations during or after exercise
- A family history of heart disease or sudden cardiac death
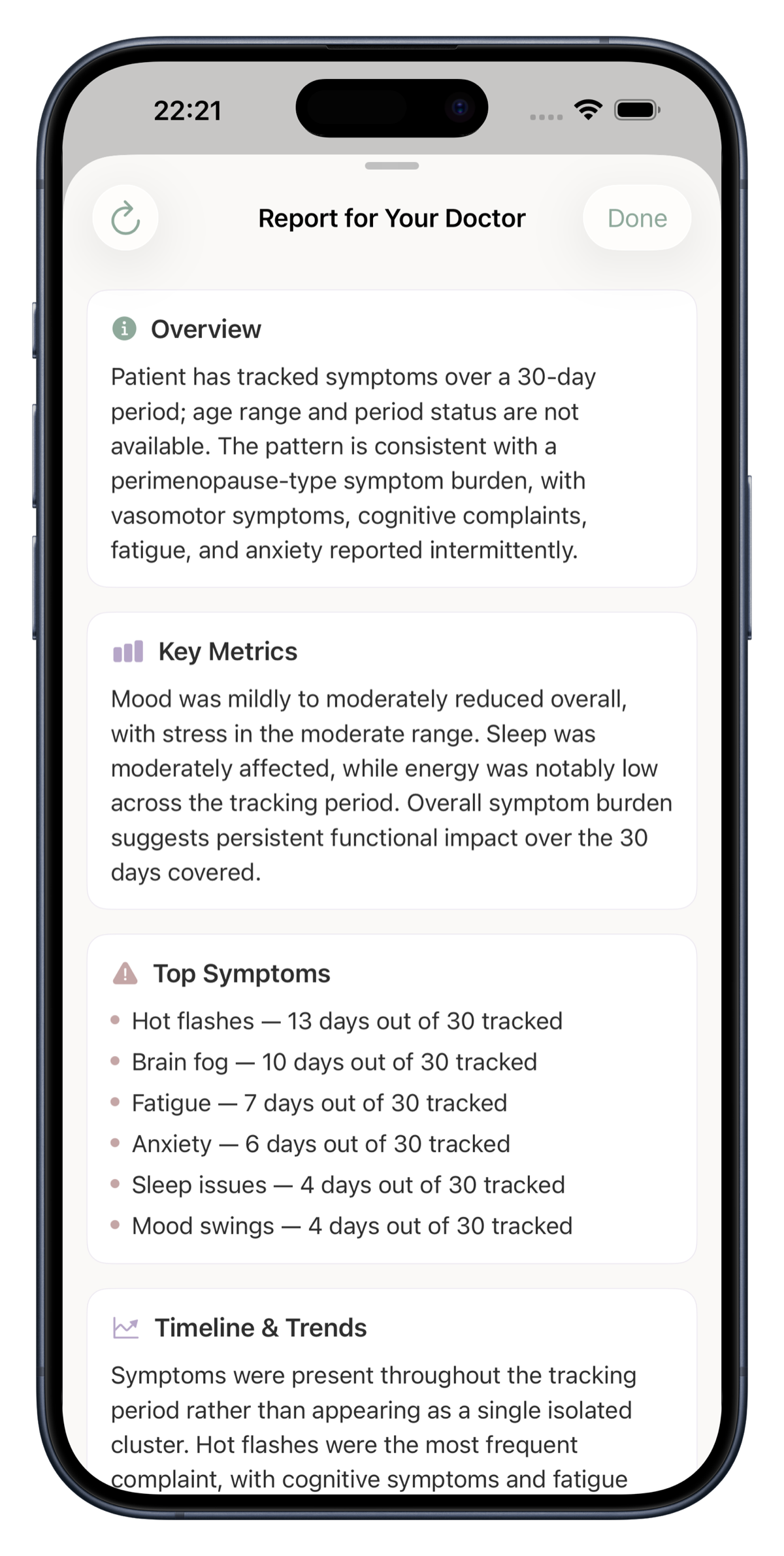
Your doctor may perform an electrocardiogram (ECG), blood tests (to check thyroid function and electrolytes), or a Holter monitor (a wearable device that records your heart rhythm over 24-48 hours). In most cases, these tests come back normal, confirming that the palpitations are hormone-related.
Benign vs. Concerning: How to Tell
This is the question that brings most women to a doctor about palpitations. The table below summarizes the patterns clinicians look for. Use it as a guide, not a diagnosis.
| Feature | Usually benign (perimenopause) | Worth a workup |
|---|---|---|
| Duration | Seconds to a couple of minutes | Sustained 10+ minutes |
| Resting heart rate | Under 100 bpm between episodes | Consistently 100+ bpm |
| Triggers | Hot flashes, caffeine, stress, late luteal phase | Exertion, lying flat, no clear trigger |
| Other symptoms | None, or mild anxiety | Chest pain, fainting, true shortness of breath |
| Pattern | Comes and goes with the cycle | Progressively worsening over weeks |
PVCs and Arrhythmia During Menopause
Premature ventricular contractions (PVCs) are the most common arrhythmia during perimenopause. A 2017 study in Menopause found that up to 47% of perimenopausal women on a Holter monitor showed PVCs — most of them entirely asymptomatic. The ones you feel are usually described as a "skipped beat," "extra thud," or "flip-flop" in the chest.
Why they spike in perimenopause: estrogen has a stabilizing effect on the cardiac electrical system. When estrogen drops or fluctuates wildly, the threshold for triggering an extra beat lowers, so the heart fires off ectopic beats more easily. PVCs that occur fewer than 10,000 times per day in an otherwise healthy heart are generally considered benign and need no treatment — but they should be quantified once with a 24- or 48-hour Holter monitor to confirm the pattern.
Other arrhythmias that get more common around menopause: atrial fibrillation (Afib), supraventricular tachycardia (SVT), and inappropriate sinus tachycardia. None are caused by perimenopause alone, but the hormonal turbulence can unmask a tendency that was always there. Any documented Afib needs a cardiologist visit — it raises stroke risk and is treatable.
Chest Pain and Chest Tightness — Is It the Heart or the Hormones?
Chest tightness and chest pain during perimenopause are common and most often not cardiac. Three patterns explain most of these episodes:
- Costochondral irritation. Estrogen affects inflammation in joint and rib cartilage. The cartilage where ribs meet the breastbone (costochondral joints) can become tender, causing a sharp or pressure-like pain that worsens with deep breathing or pressing on the spot. This is musculoskeletal, not cardiac.
- Anxiety-driven chest tightness. Perimenopause increases panic-attack frequency. The chest tightness, racing heart, and feeling of impending doom that come with a panic episode mimic a heart attack closely. Hallmark: comes with hyperventilation, peaks at 10 minutes, resolves over 30.
- Hot-flash-linked vasomotor pressure. The same blood-vessel changes that cause hot flashes can produce a transient chest pressure or "wave" sensation lasting a few minutes.
That said: chest pain on exertion, chest pain that radiates to the jaw or left arm, chest pain with sweating and nausea, or chest pain in someone with risk factors (smoking, high cholesterol, diabetes, family history) needs same-day evaluation. Women's heart-attack symptoms are often less classical than men's, and "it's probably perimenopause" should never delay a workup.
Palpitations Tied to Your Period
If you still have cycles, you may notice palpitations cluster in the few days before your period — and stop when bleeding starts. This is one of the most distinctive perimenopause palpitation patterns. The mechanism: estrogen plummets in the late luteal phase. Lower estrogen reduces vagal tone (the parasympathetic "brake" on heart rate), and the resulting sympathetic dominance triggers PACs, PVCs, and tachycardia episodes.
Why this matters: cyclical palpitations are almost always hormonal and usually improve after menopause when estrogen stops fluctuating. If yours follow this pattern, that's strong evidence the cause is endocrine, not cardiac — though a one-time cardiology workup to confirm normal anatomy is still wise.
Low Estrogen and the Heart's Electrical System
The biology behind perimenopause palpitations sits at the intersection of estrogen, the autonomic nervous system, and cardiac ion channels.
- Estrogen and vagal tone. Estrogen enhances parasympathetic (calming) activity. When it drops, sympathetic activity dominates and heart rate variability decreases — a setup for palpitations.
- Estrogen and ion channels. Estrogen modulates potassium and calcium channel function in cardiac cells. Estrogen withdrawal lengthens the QT interval slightly and can predispose to ectopic beats.
- Estrogen and blood vessels. Estrogen relaxes vascular smooth muscle. Lower estrogen leads to greater vascular reactivity — and a more reactive vascular bed means more transient heart-rate spikes after caffeine, stress, or temperature changes.
The takeaway: perimenopause palpitations are not "in your head." They are a real, measurable consequence of changing estrogen on a system that estrogen helps regulate. That's also why hormone therapy reduces palpitations for many women — it removes the trigger.
What triggers make perimenopause palpitations worse?
Understanding your triggers can help you reduce episodes. Common triggers during perimenopause include:
- Caffeine. Even if you have always tolerated coffee, your sensitivity may increase during perimenopause.
- Alcohol. Even moderate amounts can trigger palpitations, especially red wine.
- Stress and anxiety. Adrenaline directly increases heart rate and can cause arrhythmias.
- Dehydration. Low fluid intake concentrates electrolytes and affects heart rhythm.
- Poor sleep. A night of fragmented sleep significantly increases next-day palpitation risk.
- Blood sugar swings. Skipping meals or eating high-sugar foods can trigger adrenaline release that causes palpitations.
- Hot flashes. The adrenaline surge that triggers a hot flash often brings palpitations with it.
How do you manage perimenopause heart palpitations?
In the Moment
When a palpitation episode starts, these techniques can help calm it quickly:
- Vagal maneuvers. Bearing down (like you are having a bowel movement), splashing cold water on your face, or coughing forcefully can stimulate the vagus nerve and slow your heart rate.
- Slow, deep breathing. Inhale for 4 counts, hold for 4, exhale for 6. This activates the parasympathetic nervous system.
- Drink cold water. Swallowing cold water can sometimes reset heart rhythm via the vagus nerve.
- Remind yourself it will pass. Anxiety about the palpitation often prolongs it. Knowing it is a common, usually harmless perimenopause symptom helps break the anxiety-palpitation cycle.
Long-Term Strategies
- Reduce caffeine and alcohol. Try cutting back for two weeks and see if palpitations decrease.
- Stay hydrated. Aim for 8-10 glasses of water daily.
- Regular exercise. Moderate, consistent exercise strengthens the heart and improves autonomic balance. Aim for 150 minutes per week.
- Magnesium-rich foods. Magnesium supports heart rhythm. Dark leafy greens, nuts, seeds, and dark chocolate are good sources.
- Manage stress. Yoga, meditation, or progressive muscle relaxation can reduce the stress hormones that trigger palpitations.
- Protect sleep. Consistent bedtime, cool room, and limiting screens before bed all help.
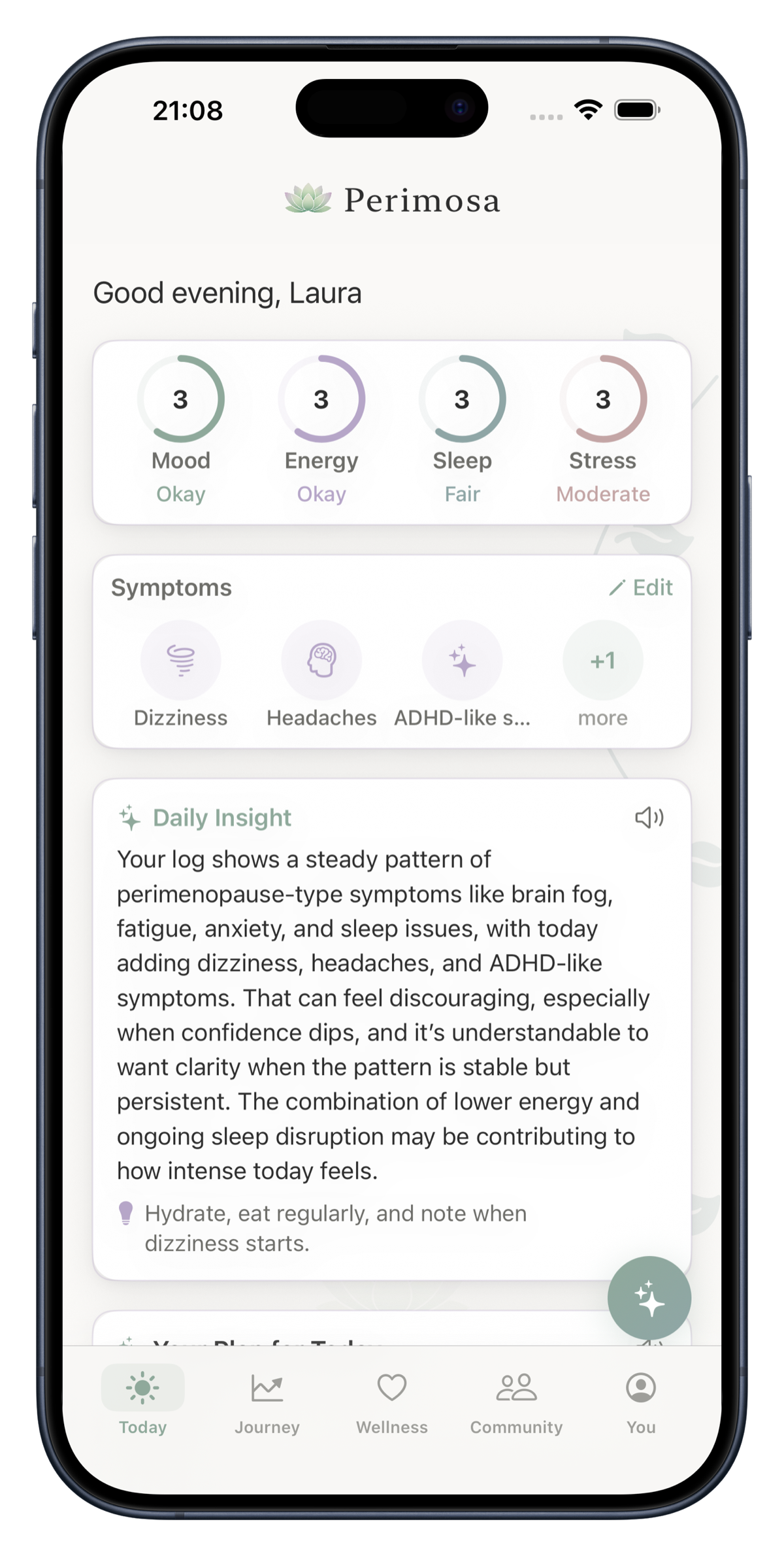
- Track your symptoms. Logging palpitation episodes alongside other daily factors like caffeine intake, sleep quality, stress, and cycle phase helps you identify your personal triggers. Perimosa makes this easy with daily check-ins that capture the full picture.
Will the Palpitations Go Away?
For most women, perimenopause-related palpitations improve significantly after menopause, when hormone levels stabilize at their new baseline. The transition can take several years, but the palpitations typically become less frequent and less intense over time.
If palpitations are significantly affecting your quality of life, discuss hormone therapy with your doctor. Stabilizing estrogen levels with HRT can reduce palpitations, hot flashes, and the anxiety that often accompanies them.
The Bottom Line
Heart palpitations during perimenopause are common, usually harmless, and driven by the same hormonal fluctuations that cause hot flashes and mood changes. They deserve medical evaluation to rule out cardiac causes, but once cleared, most women can manage them with lifestyle adjustments and trigger avoidance. Tracking when palpitations occur alongside other symptoms helps you understand your patterns and gives your doctor useful information.